
The Value of CPD Accreditation in Healthcare Training
In the ever-evolving field of healthcare, continuous professional development (CPD) is not just beneficial; it’s essential. At Meduc8ion, we understand the importance of staying up

Back in 2019, the National Health Service performed an about-face with regards to its ear wax removal services: after offering the service for years, ministers confirmed that the British Medical Association had decided it would no longer be considered part of the core services GPs were obliged to provide.
The reasons for this are multifaceted, beginning in the technical and extending to the budgetary. For years – decades, even – doctors would pump lukewarm water directly into the patients’ ear by a method commonly known as ‘syringing’ in order to flush out excess wax.
Although not entirely unsuccessful, this method suffered from two significant drawbacks, namely the lack of flow control and the lack of aim that the syringe provided.
As an essentially manual operation, it was very much up to the doctors’ degree of control whether or not the pressure was too much, and whether their aim was sufficient to avoid the eardrum (and therefore damage to it).

Thankfully, syringing has now been completely superseded by two far more precise methods: ear irrigation and microsuction. Ear irrigation is perhaps the most similar to its predecessor, in that it utilizes a small hose attached to a pump – snappily titled an ‘irrigator’ – in order to flush out the wax in much the same way, but with far greater accuracy. Microsuction varies slightly in that wax is vacuumed (rather than flushed) out.
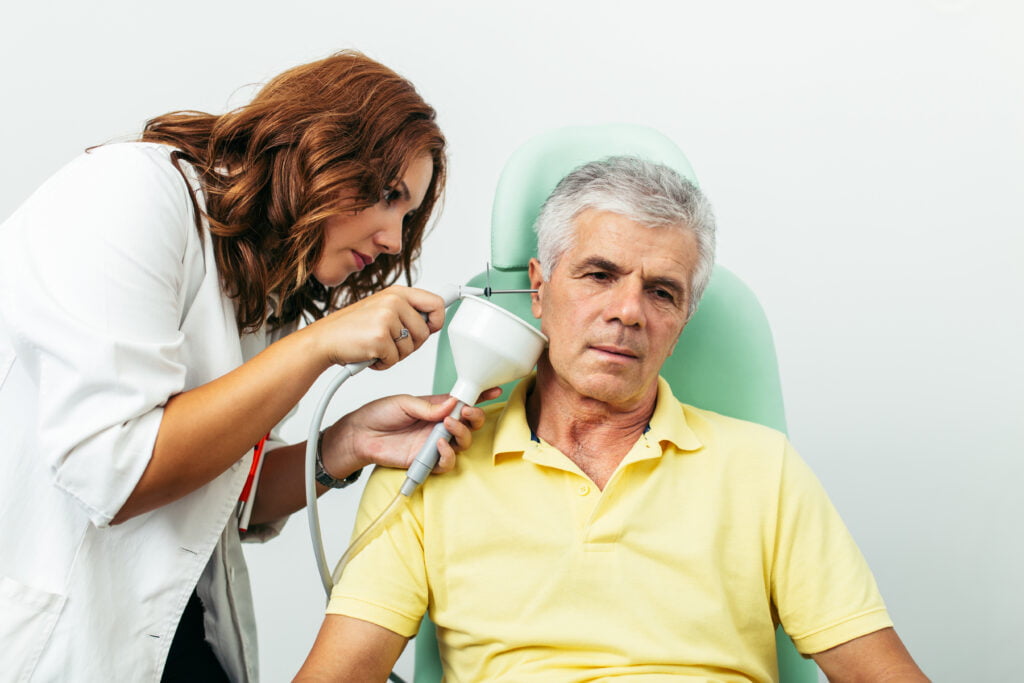
Both of these new methods are not without their costs, however, and it appears to be a cost that the NHS has thus far been unwilling to pay. As technology and methodology moved on, the health service chose to remain static in this regard, despite year-on-year budget increases peaking over the last two years as the pandemic has taken hold.
This move has caused widespread consternation among the general populace. Complaints have been made from as far afield as Spalding, Oxfordshire, Cornwall and Salisbury from patients desperate to have their wax removed. It’s not a surprise, either: some 2.3 million people per year in the UK have problems with ear wax build up.
What’s more, a lack of treatment can result in some seriously adverse effects, ranging from the annoying to the life-impeding. Among these are an irritation of the ear, earache, a ringing in the ears (tinnitus), nausea, liquid discharge/noticeable smell from the ear and dizziness. However, given enough time lacking treatment, it can result in something as grave as an overall loss of hearing.
Indeed, many people with built-up earwax find themselves unable to hear friends and colleagues as they otherwise could. This can acutely impact your day-to-day life – particularly your working life, especially if you work in a safety critical environment.
That’s why here at Meduc8ion we consider the service we provide to be so important. Not only can you help the hundreds of thousands of people up and down the country be relieved of their unfortunate predicament, but you can learn a valuable new skill as well as make some money on the side.
Our ear wax removal training course has already achieved full CPD-accreditation and had many happy coursegoers. What’s more, we’ve even had course attendees create their own small businesses as a result, and join our burgeoning network of professional Ear Wax Removal Specialists up and down the country.

Furthermore, one only has to take a glance at our sister division, Hear4U, to see the remarkable success that being a qualified and certified hearing care professional can guarantee. We pride ourselves on the help we give our communities for a reasonable price.
Now, with Meduc8ion’s fantastic courses, so can you.
To get started with your new field of expertise, simply click the link here to see course availability or why not get in touch with our expert trainer Emma on: emma@meduc8.co.uk to find out more.
The choice is yours.

In the ever-evolving field of healthcare, continuous professional development (CPD) is not just beneficial; it’s essential. At Meduc8ion, we understand the importance of staying up

Michelle Evans, a dedicated nurse based in a remote Scottish community, noticed something crucial was missing in local healthcare services: accessible, specialised ear care. Her



